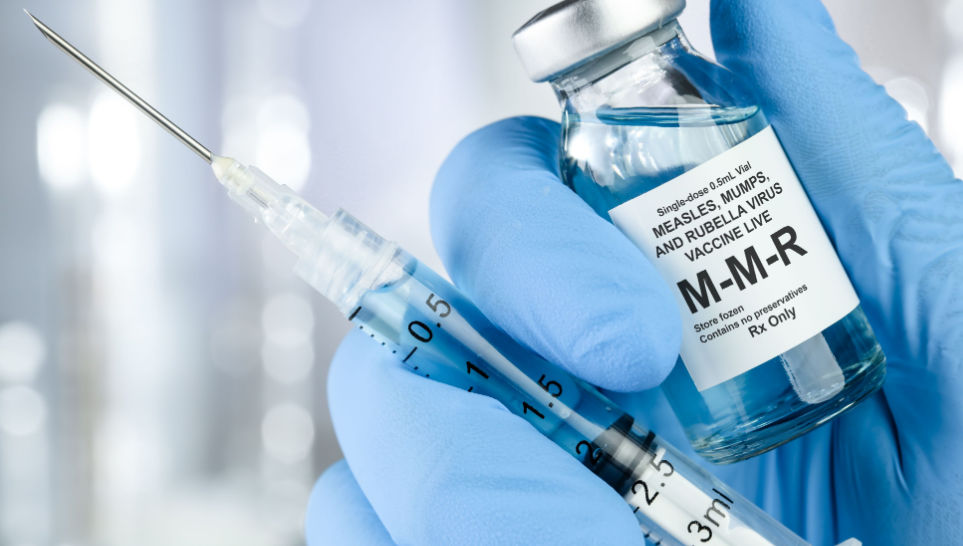
According to the Center for Disease Control and Prevention, all infants 12 months of age or older and susceptible adults who do not have documented evidence of measles immunity, such as a blood test showing the presence of measles antibody or proof of receiving 2 doses of measles vaccine, are recommended to receive the Measles, Mumps and Rubella (MMR)vaccine.
The National Network for Immunization Information website states, “Immunity against measles is particularly important for adults at high risk for measles exposure, including college students and health care workers. People born before 1957 who are not in one of these high-risk categories are generally considered immune to measles through environmental exposure. Women of child bearing age should have immunity to rubella confirmed.”
Yet as with all vaccines, it is not a one size fits all scenario. There are some instances and circumstances when it is ill advisable or contraindicated. The following information should definitely be taken into consideration before being given this vaccine.
MMR Vaccine Precaution
Any person who has had a severe reaction to gelatin or neomycin (e.g., oral or esophageal inflammation, urticaria, difficulty breathing, hypotension, shock) or a severe allergic reaction to a prior MMR immunization should only be given MMR with extreme caution.
At least six patients who were severely immunosuppressed died following administration of measles vaccine. Thus, measles vaccination is contraindicated in severe immunosuppression.
These patients may include those who have congenital immunodeficiency, HIV infection, leukemia, lymphoma or generalized malignancy or who are currently receiving alkylating agents, antimetabolites, radiation or large doses of corticosteroids.
Any proposed recipient who is experiencing a moderate or severe illness should not be vaccinated until he or she improves. However, patients with minor illnesses (e.g., upper respiratory infections with or without fever) may be vaccinated.
The CDC also advises against MMR vaccination in children if the child has moderate to severe diarrhea, moderate otitis media or moderate to severe vomiting. These contraindications remain whether or not the child has a fever.
Pregnant women should not be given MMR because of the theoretical risk of vaccine virus transmission to the fetus. Pregnancy should be avoided for one month following the monovalent measles vaccine and for three months following MMR or any other rubella-containing vaccine. However, a person in close contact with a pregnant female may receive the vaccine.
Breast-feeding is not a contraindication to MMR vaccination. It does not interfere with the response to MMR vaccine. Vaccination of a woman who is breastfeeding poses no risk to the infant being breastfed. Although it is believed that rubella vaccine virus, in rare instances, may be transmitted via breast milk, the infection in the infant is asymptomatic.
Several studies have documented the safety of measles and mumps vaccine (which are grown in chick embryo tissue culture) in children with severe egg allergy. Neither the American Academy of Pediatric’s “Red Book” Committee nor Advisory Committee on Immunization Practices consider egg allergy as a contraindication to MMR vaccine. ACIP recommends routine vaccination of egg-allergic children without the use of special protocols or desensitization procedures.