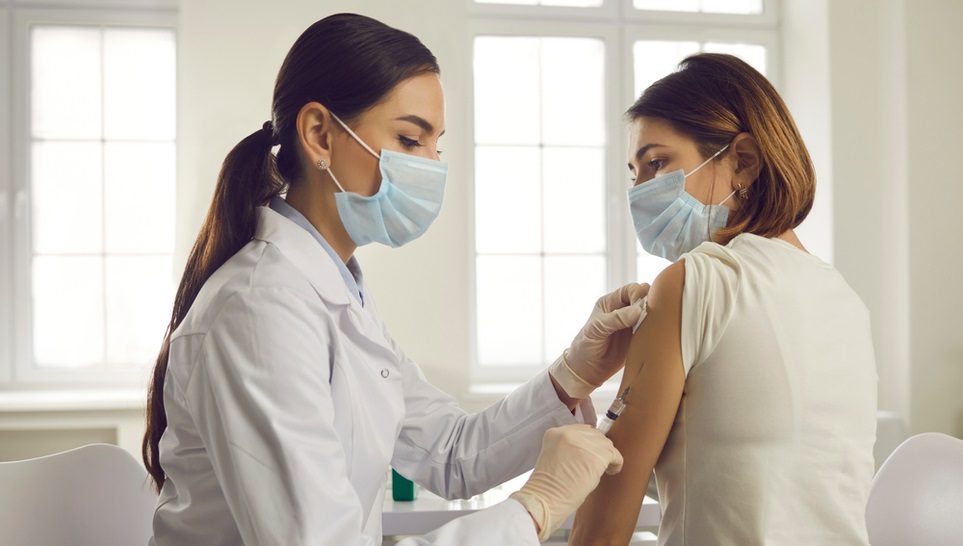
Guillain-Barre syndrome is a condition where the body attacks itself (autoimmune). In GBS the immune system attacks the body’s own nerves. Essentially the immune system begins to treat the nerves as if they were a virus or bacterium and tries to destroy them. Nerves that are attacked and destroyed are no longer able to transmit signals to the brain, resulting in tingling, numbness, and paralysis.
There are several types of Guillain-Barre syndrome, including acute motor axonal neuropathy (AMAN), acute motor-sensory axonal neuropathy (AMSAN), acute inflammatory demyelinating polyradiculoneuropathy (AIDP), and Miller Fisher syndrome (MFS). In the United States AIDP is the most common type. A small number of individuals who contract the acute form of the illness go on to suffer from the chronic form of the disease, called chronic inflammatory demyelinating polyneuropathy.
Symptoms of Guillain-Barre Syndrome
People affected by Guillain-Barre syndrome may first notice weakness and/or tingling in their fingers and toes. About 10% of the time, the sensation begins in the arms and/or face. Other symptoms may include:
- Aching or cramping pain that may get worse at night
- Back pain
- Heart and blood pressure fluctuations
- Inability to climb stairs
- Inability to move one’s eyes
- Inability to walk
- Loss of bladder or bowel function
- “Pins and needles” sensation in the extremities
- Rapid heart rate
- Slower-than-usual reflexes
- Trouble speaking
- Unsteady walking
- Unusual tiredness
- Weakness in the legs
In some cases, tingling spreads throughout the body due to the destruction of nerve cells, and if left untreated it may cause paralysis. Signs that Guillain-Barre symptoms are a medical emergency include:
- Choking on saliva
- Difficulty breathing
- Difficulty swallowing
- Rapidly-spreading tingling or weakness
- Shortness of breath when lying flat on one’s back
- Tingling that began in the feet spreading upwards throughout the body
Individuals who have any of these symptoms should seek emergency medical attention immediately. The risk of severe complications is relatively low, but in extreme cases, death from respiratory distress or heart attack is possible.
Although in some people, Guillain-Barre syndrome presents as a medical crisis and may require hospitalization, most people recover from the acute symptoms of the condition, although some continue to experience tingling and weakness in the extremities and/or fatigue. Recovery generally begins after about 2-4 weeks and may take anywhere from six months to three years.
About 5% of patients who have recovered from Guillain-Barre syndrome will experience a relapse. Children seem to be more likely to recover completely than adults. Of all people who have had Guillain-Barre syndrome, about 85% recovery completely with no lingering side effects. The sooner treatment is started, the greater the patient’s chances of complete recovery will be.
Causes
The exact cause of Guillain-Barre syndrome is unknown. The onset of the symptoms can often be correlated to a recent immunization or surgical procedure. Furthermore, individuals are more likely to experience this disorder if they have recently contracted an infectious illness such as gastroenteritis (“stomach flu”) or a respiratory infection.
Risk Factors
Males and older adults are more susceptible to Guillain-Barre syndrome than females and adults under the age of 50. Exposure (meaning that you’ve been infected with the pathogen yourself, not that you’ve been around someone else who’s been infected) to any of the following may also increase one’s risk for the syndrome:
- Campylobacter, a bacteria found most often in undercooked poultry
- Epstein-Barr virus
- Hodgkin’s lymphoma
- Human immunodeficiency virus (HIV)
- Influenza
- Mycoplasma pneumonia
- Varicella-zoster virus, the virus that causes chicken pox and shingles
If you think you may have Guillain-Barre syndrome, talk to your health care provider. Doctors diagnose Guillain-Barre syndrome by taking your medical history, and sometimes by doing testing that looks for the presence of antibodies in your blood or spinal fluid.
Learn more about Guillain-Barre syndrome.